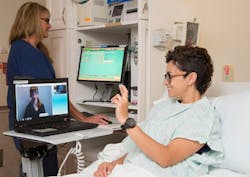
VRI at Baylor Medical Center improves patient care
One in five people in the United States speak a language other than English at home and 41% of these individuals, or 25.1 million people, are considered limited English proficient (LEP). Over the past two decades, this population has increased 15%, and by 2020, the U.S. will become the largest Spanish speaking country in the world. To address the growing needs of this population, healthcare organizations, including Baylor Scott & White, are prioritizing the need to eliminate communication barriers between patients and clinicians. Video Remote Interpreting (VRI) technology is one solution addressing the need to reduce disparities across the continuum of care. Many hospitals and healthcare systems are adopting VRI to provide clinicians with instant access to medically trained interpreters.
Baylor Scott & White is a not-for profit healthcare system in Texas and one of the largest in the United States. The system has 48 hospitals, more than 1,000 patient access points, and over 44,000 employees. Baylor University Medical Center recently implemented VRI across its health system for both LEP and deaf patients, providing access to an interpreter within seconds.
HMT spoke with Joe Valenzuela, Director of Support Services at Baylor University Medical Center who gave us more insight into VRI technology and how it’s being used at the medical center. He explained that there are five to six LEP people in the hospital each day, who previously had trouble communicating with hospital staff. The implementation of VRI has improved patient care tremendously. Doctors and patients are reaching treatment plans quicker, patients are more compliant, and community health workers are following up with them outside of the hospital to ensure they stick to the instructions they received when leaving the hospital.
Valenzuela also explained the VRI service takes into account the patient experience by offering a male or female interpreter, privacy screen, or chat feature where instructions in a targeted language are available for patients to write down if needed. The technology also allows for three different languages to be used at once, if needed (for family members of the patients to be involved in their care). Four years ago there were 14 languages available, now there are 20 with almost 24-hour coverage. If a patient speaks a language other than the 20 offered, staff members have the ability to utilize a voice-over option on the laptop/iPad devices which offers 120 spoken languages.
When we asked Valenzuela about the financial savings from VRI he told us that Baylor has been saving money while increasing quality of care and improving patient safety. The benefits go beyond financial; this technology has helped staff to communicate with patients and their loved ones, providing a powerful cure for communication gaps for LEP patients. Source: Baylor Scott & White Health
EHR-integrated post-marketing active safety surveillance program
Practice Fusion has a new program that helps alleviate the burden of adverse events reporting through the delivery of active safety surveillance messaging to healthcare providers. The post-marketing active safety surveillance program within its electronic health record (EHR) platform helps facilitate Adverse Events of Special Interest (AESI) reporting by messaging healthcare providers directly at the point of care about AESIs their patients may have experienced.
The program enables providers to monitor adverse events during patient’s treatment with prescription medications or other therapies. Using patient-level clinical characteristics, during a patient encounter, providers are notified through the Practice Fusion EHR when to screen patients for potential AESIs and how to facilitate AESI reporting following a patient encounter.
Rather than deploying a program to one medical practice at a time via the server-based model, Practice Fusion’s cloud-based model can integrate and deploy its active safety surveillance program to all practices using the company’s EHR. Practice Fusion’s connected digital health platform is used by more than 30,000 practices and has a separate de-identified clinical database, which includes more than 38 million records containing clinical data. Source: Practice Fusion
A better night’s sleep thanks to radar
We all know that sleep plays an important role in one’s physical health. While we are sleeping, there are important repairs going on in the body with the heart and blood vessels. Sleep deficiency is linked to an increased risk of stroke, heart disease, kidney disease, and high blood pressure. So why don’t we focus more on the importance of getting a good night’s rest? SleepScore Labs is looking to change that.
SleepScore Labs is a joint venture among surgeon and television host Dr. Mehmet Oz; ResMed, a leader in medical devices and digital connected care; and private equity firm Pegasus Capital Advisors, L.P., which invests in companies focused on sustainability and wellness.
S+ by SleepScore is a clinical grade nonprescription, noncontact sleep monitoring device available to the general public. Rather than covering a subject’s head, face, and body with electrodes, S+’s bio-motion sensors use refined radar to collect comprehensive and accurate data. The clinical grade technology verifies light, noise, and temperature levels in the bedroom while tracking all four stages of sleep (sleep onset, light, deep, and REM) which is then analyzed by a proprietary algorithm, giving the user a sleep score and allowing physicians to observe patterns.
HMT spoke with Colin Lawlor, CEO of SleepScore Labs who spearheaded the team that developed the S+ and brought it to market. He said, “This is the best sleep data outside of the lab.” Lawlor went on to explain that when sleep data is taken, it’s generally in the lab, where those being observed are not as comfortable as they would be in their own homes. He went on to tell HMT that the radio frequency sensor functions at 10.252 GHz. The low-power, high- frequency device scans the body every 16 seconds and can see through heavy blankets and pajamas. The backend of the comprehensive device collects data and gives advice to the individual using S+ so they’ll know if they have to visit a sleep lab or change some of their habits.
Lawlor went on to tell HMT that those who used S+ for more than one week saw 31 more minutes of sleep per night in comparison with those who use medications who only see eight more minutes of sleep per night. Source: SleepScore Labs
Introducing Elon Musk’s latest venture—neural lace
Neural lace could be the next step in human and computer advancement
Neural lace made headlines with Elon Musk launching Neuralink, a medical research company that aims to merge the human brain with intelligent computers. And while this sounds like it’s pulled from the pages of a Sci-Fi novel, neural lace could be the next advancement in the field of AI.
What is neural lace?
At its most basic form, neural lace is an ultrathin mesh that can be implanted in the skull, forming a collection of electrodes capable of monitoring brain function. It creates an interface between the brain and the machine. To insert neural lace, a tiny needle containing the rolled up mesh is placed inside the skull and the mesh is injected. As the mesh leaves the needle it unravels, spanning the brain. Gradually, the lace will be accepted as part of the brain and will even move with it as it grows or very slightly changes size. Researchers working with neural lace have tested the mesh-like structure on live mice with few negative impacts reported once full autopsies have been performed.
What can neural lace be used for?
It’s thought that neural lace could treat neurodegenerative disorders such as Parkinson’s disease and other life-altering brain disorders. According to The Smithsonian, neural lace could be used by the U.S. military, via the U.S. Air Force’s Cyborg cell program, ‘which focuses on small-scale electronics for the performance enhancement of cells’.
Similar practices could help people with missing limbs use ‘connected’ artificial body parts unassisted, using only brain power. Neural lace could potentially help someone with a neurodegenerative condition regain their ability to eat, walk, and even talk.
Neuroscience startup Kernel hopes to produce widely available implants that sufferers of neurological conditions such as Parkinson’s and Alzheimer’s disease can buy.
Engineers at Kernel, which was founded in 2016, want to better understand the human brain and why brain cells fail, causing chronic neurodegenerative diseases. Its founder Bryan Johnson has committed more than $100 million of his own money to create interfaces between humans and computing devices.
In an interview with The Verge, Johnson said, “We know if we put a chip in the brain and release electrical signals that we can ameliorate symptoms of Parkinson’s. This has been done for spinal cord pain, obesity, anorexia … what hasn’t been done is the reading and writing of neural code.”
But while its benefits appear obvious in the medical field, beyond that the possibilities of mapping brain activity and even thoughts could see the relationship between human and machine get a lot closer. Ultimately, neural lace could enable people to communicate with computers, even making it possible to upload or download thoughts to and from an intelligent computer. If the mesh is inserted and accepted by the brain, the brain would essentially be able to wirelessly connect to a computer, providing an interface between your brain and a computer.
What is Elon Musk’s Neuralink?
Musk has a well-documented history with artificial intelligence. In September 2016, Musk, along with Reid Hoffman, Jessica Livingston, Peter Thiel, and others gave support to OpenAI, a non-profit AI research organization working toward ‘friendly AI’. Open AI’s friendly AI is essentially artificial intelligence that will benefit humans and create a standardized approach to AI creation and deployment.
Neuralink is Musk’s latest venture, and according to The Wall Street Journal, it aims to connect computers to your brain through the use of neural lace. It is suggested that Musk wants to ensure that humans can keep up with technology in the midst of rapid AI development. This isn’t the first time Musk has mentioned neural lace, having previously stated that it could stop humans from becoming house cats to artificial intelligence. Source: techworld